Neurology: Demyelinating Diseases: Multiple Sclerosis. Acute – Flashcards
Unlock all answers in this set
Unlock answersquestion
What is multiple sclerosis (MS)?
answer
It is an immune-mediated inflammatory disease that attacks myelinated axons in the CNS, destroying the myelin and the axon in variable degrees and producing significant physical disability
question
Question: what is the etiology of multiple sclerosis?
answer
Unknown
question
What are the 2 reasons for the disease?
answer
1. *Genetic susceptibility* & 2. *Environmental factors*: i. Infections (the virus can influence on nervous system directly or through the autoimmune mechanisms). ii. Geographical (groundwater properties, the number of light days in a year) iii. Toxins iv. Social conditions v. Diet (dominating meat in the diet) vi. Other factors (trauma).
question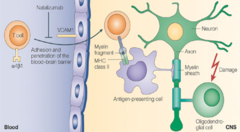
what is the pathogenesis of multiple sclerosis?

answer
The mechanism of demyelination in multiple sclerosis may be activation of myelin-reactive T cells in the periphery, which then express adhesion molecules, allowing their entry through the blood-brain barrier (BBB). T cells are activated following antigen presentation by antigen-presenting cells such as macrophages and microglia, or B cells. Perivascular T cells can secrete proinflammatory cytokines, including interferon gamma and tumor necrosis factor alpha. Antibodies against myelin also may be generated in the periphery or intrathecally. Ongoing inflammation leads to epitope spread and recruitment of other inflammatory cells (ie, bystander activation). The T cell receptor recognizes antigen in the context of human leukocyte antigen molecule presentation and also requires a second event (ie, co-stimulatory signal via the B7-CD28 pathway, not shown) for T cell activation to occur. Activated microglia may release free radicals, nitric oxide, and proteases that may contribute to tissue damage
question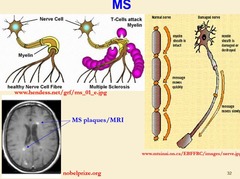
Question: what is the classification of multiple sclerosis (MS)?

answer
1. Relapsing-remitting. 2. Primary progressive. 3. Secondary progressive. 4. Relapsing progressive. 5. Benign. 6. Spinal form. 7. Neuromyelitis optica (Devic disease). 8. Marburg variant.
question
What is a Benign MS?
answer
No disability w/ return to Normal b/w attacks.
question
What is a Relapsing-remitting MS[RRMS]?
answer
Unpredictable attacks Which may possibly leave permanent deficits, followed by periods of Remission.
question
What is a Primary progressive MS[PPMS}?
answer
Steady Increase of Disability w/o attacks.
question
What is a Secondary progressive. MS[SPMS]?
answer
Initial Relapsing-Remitting MS that suddenly begins to decline w/o periods of Remission.
question
What is a Progressing Relapsing MS[PRMS]?
answer
Steady Decline since disease onset w/ superimposed attacks.
question
Name the clinical forms of *Multiple Sclerosis*?
answer
1. Cerebral : * cortical [epileptic attacks, psychiatric disorders] Visual* brainstem *Cerebellar. 2. Spinal: *Cervical *Thoracic *lumbar - *sacral* pseudo exacerbation. 3. Cerebrospinal
question
Question: what is the classification of multiple sclerosis according to the periods?
answer
*Exacerbation* *Remission (complete, incomplete)*. *Stable period*
question
Question: what is the classification of multiple sclerosis according to the course?
answer
1. Acute. 2. Subacute. 3. Chronic: - Remittent,. - Remittent - progressive. - Progressive - remittent. - Progressive.
question
Question: what is the classification of multiple sclerosis according to the degree?
answer
1. I - patient has difficulty to walk only after physical training. 2. II - patient has difficulty to walk and weakness on 2-3 km. 3. III - patient has spastic-paretic gait, difficulty to walk and weakness on 200-300 m. 4. IV - patient can't walk without help. 5. V - patient can't walk or has blindness. *OVERALL MS Sx SHOULD LAST FOR 24 HOURS*.
question
Question: what is the clinical presentation of multiple sclerosis?
answer
1. Sensory disorders (Paresthesia). It is the feeling of numbness or tingling in one of the extremity. i. Subjective sensory disturbances are early signs of MS ii. Then conductive sensory disorders are joined to them iii. Muscle - joint sense usually suffers at the fifth year of the disease and later iv. The loss of vibration sense points on posterior columns lesion 2. Motor disorders - weakness in lower extremities. This symptom is much more common at the age of 25 - 40 years. Hemiparesis, lower paraparesis and monoparesis 3. Brainstem disorders: i. dizziness ii. nystagmus iii. vestibular ataxia; iv. Sometimes trigeminal pains are observed 4. Retrobulbar neuritis is a progressive loss of vision, color vision disturbances. It lasts for about several weeks 5. Oculomotor n. disorders (diplopia and cross eye) 6. Pelvis disorders (retention of urine, micturition) 7. Acute vestibular syndrome 8. Cerebellar disorders - ataxia, disorders of coordination (Dysmetria, hypermetria, Intention tremor, Asynergy) 9. Nonspecific symptoms: i. General weakness ii. Cognitive disorders iii. Memory iv. Attention disturbances v. Behavioral disorders vi. Depression, euphoria and fatigue syndrome
question
Question: what is the principle of Dx of multiple sclerosis?
answer
1. Immune examinations of blood and CSF. Usually there are increased IgG, M, and A contents. 2. Insignificant increase of protein contents and moderate pleocytosis*[WBC]* in CSF. 3. Lymphocytosis, eosinophilia - in exacerbation stage; leukopenia, lymphopenia - in the period of remission. 4. Increased thrombocytes aggregation and fibrinogen contents. 5. Increased IgG contents in serum and decreased T - lymphocytes quantity.
question
How the diagnosis of multiple sclerosis made by criteria?
answer
The diagnosis of multiple sclerosis is made by this criteria: 1. Patient should have at least 2 focuses of lesion and 2 exacerbations, or 2 exacerbations of 1 clinical focus and 1 paraclinical supposed focus. 2. There should be at least 3 focuses in MRI (2 of them should be located paraventricular, 1 - subtentorial (that means in brainstem or cerebellum). The diameter of focuses should be at least 6 mm, or there should be 4 focuses, 1 of them periventricular.
question
How many therapies exist for now for MS? Disease modifying therapies in the market
answer
9 FDA approved MS Therapies. 1 of them is not being used bec of many SDx. Reduces relapses Reduce progression of disabilities. Reduce new lesions seen in the MRI.
question
What is the FDA Approved treatment of Injectable Therapies for multiple sclerosis? Interferon Beta-1b
answer
*Interferon Beta-1b*: BETASERON/EXTAVIA Lowers the T-Cell Trafficking across BBB . 8 mlU SubQ every other day. Approved for RRMS, 30% effective. SDx: *Flu like Symptoms*
question
What is the FDA Approved treatment of Injectable Therapies for multiple sclerosis? Interferon Beta-1a AVONEX
answer
* Interferon Beta-1a*: AVONEX/REBIF Slows the crossing of T-cells across the BBB. *AVONEX*: 30 Micrograms IM Weekly * Reduces Relapses* *Slows Rate of Disability Progression* *Reduce MRI Lesions Burdon* SDx: Flu Like symptoms, Needs Blood /Liver Monitoring.
question
What is the FDA Approved treatment of Injectable Therapies for multiple sclerosis? Interferon Beta-1a REBIF
answer
*REBIF* *22-44 MicroGram SubQ 3x/week * Reduces # & severity of Relapses. * Delays Disability* *Reduces MRI Lesion* Burden.
question
What is the FDA Approved treatment of Injectable Therapies for multiple sclerosis? GLATIRAMER aCETATE*: COPAXONE
answer
*GLATIRAMER aCETATE*: COPAXONE *20 mg SubQ daily. * Polymer of 4 AA found in Myelin, that Suppress the T-Cells and Mods. the Immune system. Reduces Inflammation. *Approved for RRMS* * Reduces the Freq of Relapses. * Does not Reduce the Disability. * Safe in Pregnancy. * 1 SubQ/Day Shot. *SDx: No Side effects.
question
What is the FDA Approved treatment of Injectable Therapies for multiple sclerosis? *Tysabri*: [NATALIZUMAB]
answer
*Tysabri*: [NATALIZUMAB]: Monoclonal Abx that blocks the receptors on WBC and prevents them from crossing BBB. * 300mg IV , 1x / Mo. IV inFusion. *TOUCH Protocol* * Reduces relapses by 67%* * Slows Disability Progression* *Reduce MRI Lesions Burdon* * Risk of PML* Also used in Ulceritis.
question
What is a PML ?
answer
PML: Stands for progressive multifocal leukoencephalopathy, a rapidly progressive, often fatal viral infection of the brain. Commonly abbreviated as PML. PML is believed to be due to the *Jacob-Creutzfeldt (JC) papovavirus*. The virus infects oligodendrocytes (support cells in the brain).
question
What is the FDA Approved treatment w/ Pills for multiple sclerosis?
answer
*FINGOLIMOD[GILENYA]* *TERIFLUNOMIDE [AUBAGIO]* *DIMETHYL FUMARATE[TECFIDERA]*
question
What is the FDA Approved treatment w/ Pills for multiple sclerosis? *FINGOLIMOD[GILENYA]*
answer
*APPROVED IN 2010.* *REDUCED RELAPSES BY APPROX. 50%* *REDUCED DISEASE PROGRESSION* *Reduce MRI Lesions Burdon* BELIEVED TO LIMIT THE MIGRATION OF LYMPHOCYTES FROM THE LYMPH NODES. *SDx: Need to monitor for Cardiac side effects.[Sudden Cardiac Deaths]* * Ophthalmologic Exam, monitor for MAcular degeneration* *Blood Monitoring for Zoster or Shingle Virus*
question
What is the FDA Approved treatment w/ Pills for multiple sclerosis?TERIFLUNOMIDE [AUBAGIO]*
answer
*APPROVED SEPT, 2012* * 7mg, 14mg 1x/day oral* *REDUCES ACTIVATED LYMPHOCYTES IN CNS* *IMMUNOMOD. W/ ANTI-INFLAMMATORY AGENT* *80% ReducTION IN NEW BRAIN MRI Lesions * *REDUCED RELAPSES BY APPROX. 30%* *REDUCED DISEASE PROGRESSION, 30%* SDx: * BLOOD mONITORING* *PREG: X-CATEG.* *BP MONITORING* *TB TEST*
question
What is the FDA Approved treatment w/ Pills for multiple sclerosis? *DIMETHYL FUMARATE[TECFIDERA*
answer
*APPROVED MARCH, 2013* 240 mg 2x/day. *REDUCED ANNUAL RELAPSES BY APPROX. 53%* * REDUCE Disability Progression by 38%* *ReducTION IN NEW BRAIN MRI Lesions * MOA: Believed to have an anti oxidant effect and inhibit pro-inflammatory immune pathway. * Favorable Side Effects* FLUSHING FOR AN HOUR AFTER ADMINISTERING THE MEDx. U GET USED TO IT.
question
Question: what is Acute multiple encephalomyelitis (AMEM)?
answer
It is an infectious - allergic disease characterized by acute multiple lesion of the brain and spinal cord
question
Question: what are the clinical forms of Acute multiple encephalomyelitis (AMEM)?
answer
1. Encephalomyelopathy Radiculoneuritis - it is the most common form of the disease, which is characterized by the lesion of all parts of nervous system. 2. Polioencephalomyelitis - it is characterized by the lesion of CN's nuclei and spinal cord gray substance. 3. Optical Encephalomyelitis and optic myelitis - are characterized by optic nerve neuritis and symptoms of lesion of brain and spinal cord. 4. Disseminated myelitis - the spinal cord is damaged on different levels.
question
Question: what is the treatment of Acute multiple encephalomyelitis (AMEM)?
answer
1. Corticosteroids: Prednisolone and Methylprednisolone in dose 10 - 15 mg per kg i/v by drops per day. Later we can use it in pills - 1.5 - 2 mg/kg every other day. 2. Together with this medicine we prescribe anabolics, K, Ca, vitamin C. 3. In acute stage we prescribe desensibilization and dehydrating medicines. In case of severe bulbar disorders we include resuscitation measures. 4. Plasmapheresis and vitamin B are also used. 5. In residual period we prescribe massage, dibazol, KJ, biostimulants, Lidasa, Seduxen, sanatorium treatment.
question
Question: what is the principle of treatment of multiple sclerosis?
answer
A. Pathogenetic treatment *1. Corticosteroids and ACTH* i.* Prednisone* is used orally 1 - 1.5 mg/kg/day twice a day during 10 - 14 days. Then during the next 2 months we decrease the dose gradually. OR ii. One of the most popular schemes for *Methylprednisolone* usage is 500 - 1000 mg per day i/v in 500 ml of physiological solution during 3 - 5 days. Then Prednisone is used in dose 0.5 - 1 mg/kg during 3 - 7 days with gradually decreasing of dose during the next 2 - 3 weeks. This way of usage has much more expressed and quick effectiveness and insignificant outside effects OR iii. *Dexamethasone* is used i/v or i/m according to the scheme - 8 mg per day during 7 days, 4 mg - 4 days, 2 mg - 3 days. It is used at retrobulbar neuritis OR iv. ACTH has immune suppressive activity, inhibits cellular and humoral immunity. It is used in dose 40 - 100 U i/m during 10 - 14 days. v. *Plasmapheresis* is used in case of exacerbation. 2. Cytostatic and immune modulators, nonspecific immune suppressors i. *Azathioprine, Cyclophosphamide, Cyclosporine* ii. The representatives of immune modulators are - T - activin, Timalin, Myelopid, Levamisole. They are prescribed at progressive forms of MS. iii. *T - Activin*is used in dose 100 mcg s/c every evening during 5 days, then 1 - 3 injections every 10 days. iv. *Timalin* is used in dose 10 mg i/m twice a day during 5 days, then every 10 days 2 injections are used. 3.* Cytokines, interferon* i. There are 3 types of Interferon - α, β, γ. ii. α - Interferon has neither toxic nor treating activity. iii. γ - Interferon activates immune system and that's why it provokes exacerbations. iv. β - Interferon inhibits production of γ - interferon, increases activity of T - suppressors, has antiproliferative, antiviral and immune modulating properties. v. *Rebif *- is a modern human β - interferon produced by "Serono" production. It is used in dose 6 - 12 mln s/c 3 times per week. It is one of the most effective modern medicines in MS patients, but unfortunately it is very expensive 4. Antigen - specific immune therapy i. *Copaxone*: 20 mg per day s/c during 6 - 24 months. It has selective immune modulating action. B. Other treatment: Vitamins B group Desensibilization medicines Amino acids * Nootropics* ATP, Cocarboxylase Biostimulants Entero and hemosorption Antiplatelet Antioxydants Angioprotectors Inhibitors of proteolytic enzymes Regeneration stimulants
question
Question: what is Amyotrophic lateral sclerosis?
answer
It is a chronic progressive disease of nervous system and is defined pathologically as one in which there is degeneration of both upper and lower motor neurons of brain and spinal cord.
question
Question: what is the etiology of Amyotrophic lateral sclerosis (ALS)?
answer
Unknown
question
What is the main reasons of ALS development?
answer
1. Insufficiency of spinal blood circulation. 2. Vertebrogenic pathology 3. Trauma 4. Infections 5. Demyelination 6. Metabolic disorders 7. Tumours (rarely) 8. Radiation
question
Question: what is the classification of ALS?
answer
There are 3 forms of the disease: 1. Classical or sporadic ALS 2. Familial ALS [inherited as autosomal dominant and autosomal recessive one],associated with: · Dementia. · Extrapyramidal disorders. · Extrapyramidal and cerebellar disorders. · Extrapyramidal and sensory disorders. · Peripheral neuropathy. Familial ALS usually begins at the age of 45 - 48. 3. Complex - ALS - Parkinson disease - Dementia
question
what are the clinical forms of ALS?
answer
1. Cerebral i. spastic tetraparesis ii. Pseudobulbar syndrome. iii. Extrapyramidal nervous system (the signs of Parkinson disease) and iv. Cortex of frontal lobe (the signs of Dementia) is involved. 2. Bulbar[Bulbar palsy refers to impairment of function of the cranial nerves IX, X, XI and XII, which occurs due to a lower motor neuron lesion either at nuclear or fascicular level in the medulla oblongata or from lesions of the lower cranial nerves outside the brainstem.] i. lesion of cranial nerves of IX, X, XI, XII CN's that leads to the classic bulbar syndrome 3. Cervical - thoracic i. Weakness of proximal muscles and later distal parts of the upper extremities. ii. well - expressed hypotrophy, iii. increased muscle tone according to the spastic type iv. hyperreflexia, v. Pathologic signs. 4. Lumbar - sacral
question
Question: what is Transverse myelitis?
answer
It is a syndrome characterized by acute spinal cord dysfunction involving both halves of the cord in transverse section.
question
Question: what is the etiology of Transverse myelitis?
answer
1. Congenital—vascular malformation 2. Infectious—viral infection 3. Autoimmune—peri-infectious, post infectious, or vaccinal myelitis 4. Multiple sclerosis 5. Neoplastic—paraneoplastic necrosis 6. Toxic—secondary to heroin injections 7. Vascular—vascular insufficiency—arteritis, dissecting aneurysm, aorta resection, aortic aneurysm 8. Degenerative—irradiation 9. Idiopathic
question
Question: what is the clinical presentation of transverse myelitis?
answer
1. Paresthesias, which are often described as numbness, tingling, or pins and needles, usually begin in the toes or the feet and extend up the lower limbs into the trunk, with eventual involvement of the upper limbs in cervical transverse myelitis. 2. Pain is of sudden onset, usually severe and corresponding to the level of the cord involvement. Consequently, the pain is often in the interscapular region. 3. Progressive lower limb weakness is noted, often presenting with "stumbling or weakness of one leg." 4. Urinary retention occasionally occurs as the initial complaint and is usually followed by lower limb weakness in a short period of time.
question
Question: what is the diagnostic procedure of transverse myelitis?
answer
1. MRI scan shows areas of increased signal intensity involving gray matter and surrounding white matter. 2. Electromyography performed after 2 weeks will demonstrate motor axonopathy in keeping with anterior horn cell involvement. 3. Lumbar puncture. The CSF is abnormal with a pleocytosis, The cells are predominantly monocytic. Protein content is elevated.



