Neurology – Charts – Flashcards
Unlock all answers in this set
Unlock answersquestion
CNS : *Cerebral Cortex Lesion* : Motor Findings
answer
- chronic contralateral corticospinal-type weakness and spasticity - flexion is stronger than extension in the arm - plantar flexion is stronger than dorsiflexion in the foot, and the leg is externally rotated at thehip
question
CNS : *Cerebral Cortex Lesion* : Sensory Findings
answer
Contralateral sensory loss in the limbs and trunk on the same side as the motor deficits
question
CNS : *Cerebral Cortex Lesion* : DTRs
answer
increased DTRs
question
CNS : *Cerebral Cortex Lesion* : example of cause
answer
cortical stroke
question
CNS : *Brainstem Lesion* : Motor Findings
answer
weakness and spasticity plus cranial nerve deficits such as diplopia and dysarthria
question
CNS : *Brainstem Lesion* : Sensory Findings
answer
variable; no typical sensory findings
question
CNS : *Brainstem Lesion* : DTRs
answer
increased DTRs
question
CNS : *Brainstem Lesion* : Example of Cause
answer
brainstem stroke, acoustic neuroma
question
CNS : *Spinal Cord Lesion* : Motor Findings
answer
weakness and spasticity affecting both sides causing paraplegia or quadriplegia depending on the level of injury
question
CNS : *Spinal Cord Lesion* : Sensory Findings
answer
dermatomal sensory deficit on the trunk bilaterally at the level of the lesion and sensory loss from tract damage below the level of the lesion
question
CNS : *Spinal Cord Lesion* : Deep Tendon Reflexes
answer
increased DTR
question
CNS : *Spinal Cord Lesion* : examples of causes
answer
trauma, causing cord compression
question
CNS : *Subcortical Gray Matter* : Basal Ganglia Lesion : Motor Findings
answer
slowness of movement (bradykinesia), rigidity, and tremor
question
CNS : *Subcortical Gray Matter* : Basal Ganglia Lesion : Sensory Findings
answer
sensation not affected
question
CNS : *Subcortical Gray Matter* : Basal Ganglia Lesion : Deep Tendon Reflexes
answer
DTR normal or low
question
CNS : *Cerebellar Lesion* : Motor Findings
answer
hypotonia, ataxia, and other abnormal movements, including nystagmus, dysdiadochokinesis, and dysmetria
question
CNS : *Cerebellar Lesion* : Sensory Findings
answer
sensation not affected
question
CNS : *Subcortical Gray Matter* : Basal Ganglia Lesion : Examples of Causes
answer
parkinsonism
question
CNS : *Cerebellar Lesion* : Deep Tendon Reflexes
answer
DTR normal or decreased
question
CNS : *Cerebellar Lesion* : examples of causes
answer
cerebellar stroke, brain tumor
question
PNS : *Anterior Horn Cell Lesion* : Motor Findings
answer
weakness and atrophy in a segmental or focal pattern; fasiculations
question
PNS : *Anterior Horn Cell Lesion* : Sensory Findings
answer
sensation intact
question
PNS : *Anterior Horn Cell Lesion* : Deep Tendon Reflexes
answer
DTR decreased
question
PNS : *Anterior Horn Cell Lesion* : Examples of Causes
answer
polio, amyotrophic lateral sclerosis
question
PNS : *Spinal Roots and Nerves Lesions* : Motor Findings
answer
weakness and atrophy in a root-innervated pattern; sometimes with fasiculations
question
PNS : *Spinal Roots and Nerves Lesions* : Sensory Findings
answer
corresponding dermatomal sensory deficits
question
PNS : *Spinal Roots and Nerves Lesions* : Deep Tendon Reflexes
answer
decreased DTRs
question
PNS : *Spinal Roots and Nerves Lesions* : Examples of Causes
answer
herniated cervical or lumbar disc
question
PNS : *Peripheral Nerve - Mononeuropathy* : Motor Findings
answer
weakness and atrophy in a peripheral nerve distribution; sometimes with fasiculations
question
PNS : *Peripheral Nerve - Mononeuropathy* : Sensory Findings
answer
sensory loss in the pattern of that nerve
question
PNS : *Peripheral Nerve - Mononeuropathy* : Deep Tendon Reflexes
answer
decreased DTR
question
PNS : *Peripheral Nerve - Mononeuropathy* : examples of causes
answer
trauma
question
PNS : *Peripheral Nerve - Polyneuropathy* : Motor Findings
answer
weakness and atrophy more distal than proximal; sometimes with fasiculations
question
PNS : *Peripheral Nerve - Polyneuropathy* : Sensory Findings
answer
sensory deficits, commonly in stocking-glove distribution
question
PNS : *Peripheral Nerve - Polyneuropathy* : Deep Tendon Reflexes
answer
decreased deep tendon reflexes
question
PNS : *Peripheral Nerve - Polyneuropathy* : Examples of Causes
answer
peripheral polyneuropathy of alcoholism, diabetes
question
PNS : *Neuromuscular Junction Lesion* : Motor Findings
answer
fatigability more than weakness
question
PNS : *Neuromuscular Junction Lesion* : Sensory Findings
answer
sensation intact
question
PNS : *Neuromuscular Junction Lesion * : Deep Tendon Reflexes
answer
normal DTRs
question
PNS : *Neuromuscular Junction Lesion* : Examples of Causes
answer
Myasthenia Gravis
question
PNS : *Muscle Lesion* : Motor Findings
answer
weakness usually more proximal than distal; fasiculations rare
question
PNS : *Muscle Lesion* : Deep Tendon Reflexes
answer
normal or decreased DTRs
question
PNS : *Muscle Lesion* : Examples of Causes
answer
muscular dystrophy
question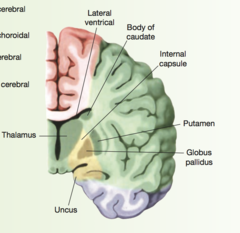
Anterior Cerebral Artery

answer
pink part
question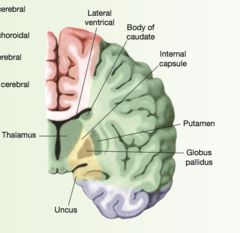
Anterior Choroidal Artery

answer
yellow part
question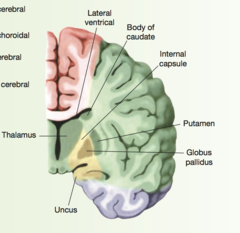
Middle Cerebral Artery

answer
green part
question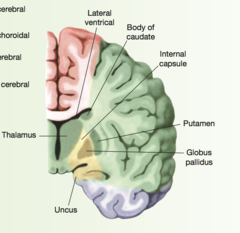
Posterior cerebral artery

answer
purple part
question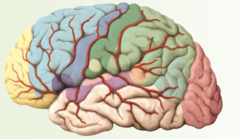
Prefrontal area

answer
yellow part
question
Premotor area
answer
light blue part
question
Primary Motor Cortex
answer
light purple area
question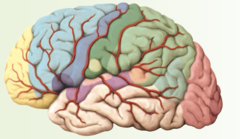
Motor speech (Broca's) area

answer
dark purple area
question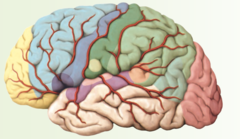
Primary Somatic Sensory Cortex

answer
Dark Green area
question
Somatic Sensory Association Area
answer
Middle green area
question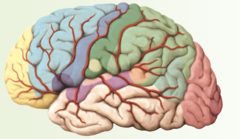
Taste area

answer
yellowish green area
question
Primary Auditory Cortex
answer
light pinkish area
question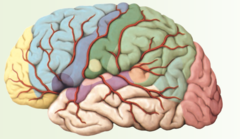
Auditory Association Area

answer
Violet area
question
Sensory Speech (Wernicke's area)
answer
orange area
question
Reading comprehension area
answer
teal area
question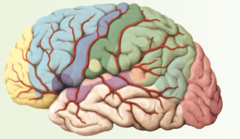
Visual association area

answer
middle pink area
question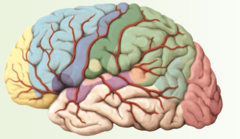
Visual cortex

answer
red area
question
Vasodepressor or Vaovagal Syncope
answer
- sudden peripheral vasodilation esp in skeletal muscles without compensatory risk in cardiac output; heart rate then blood pressure fall; often slow onset, slow offset - brought on by a strong emotion such as fear or pain - predisposing factors : fatigue, hunger, a hot humid environment are - prodromal manifestations : restlessness, weakness, pallor, nausea, salivation, sweating, yawning - prompt return of consciousness when lying down but pallor weakness nausea and slight confusion may persist for a time
question
Orthostatic (Postural) Hypotension
answer
- Inadequate vasocontrictor reflexes in both arterioles and veins, with resultant venous pooling, decreasing cardiac outpat, and low blood pressure - brought on by standing up - parkinsons, shy-drager syndrome, lewy body disease diabetes, amyloidosis, antihypertensive vasodilator drugs; prolonged bed rest are predisposing factors - associated with light headdedness and palpitations on standing up - improvement with lying down
question
Cough Syncope
answer
- neurally mediated, possible vagal stimulation - brought on by severe paroxysm of coughing - chronic bronchitis in a muscular man is a predisposing factor - no prodromal manifestations except for cough - prompt return to normal
question
Micturation Syncope
answer
- vasovagal stimulation - brought on by emptying the bladder after getting out of bed to void - predisposing factors include nocturia - prompt return to normal
question
Arrhythmias
answer
- decreased cardiac output from cardiac ischemia, ventricular arrhythmias, prolonged QT syndrome, persistent bradycardia, infrafasicular block; often sudden onset; sudden offset - precipitating factors include sudden change in rhythm - predisposing factors include heart disease, aging decrease tolerance of abnormal rhythms - prompt return to normal prolonged cerbral hypoperfusion cardiac arrest
question
Aortic Stenosis and Hypertrophic Cardiomyopathy
answer
- vascular resistance falls with exercise, but cardiac output cannot rise due to outflow obstruction - precipitating factors include exercise - predisposing factors include cardiac disorders - usually prompt return to normal
question
Myocardial Infarction
answer
- sudden arrhythmia or decreased cardiac output - predisposing factors include coronary artery disease - prodromal manifestation is ischemic chest pain
question
Massive Pulmonary Embolism
answer
- sudden hypoxia or decreased cardiac output - variable precipitating factors including prolonged bed rest and clotting disorders - DVT, bedrest, hypercoagulable states (SLE; cancer), protein S or C deficiency, antithrombin III deficiency, estrogen therapy - dyspnea, pleuritic chest pain are prodromal manifestations - recovery is related to time to diagnosis and treatment
question
Hypocapnia due to Hyperventilation
answer
- constriction of cerebral blood vessels secondary to hypocapnia induced by hyperventilation - precipitating factors : anxiety and panic disorders - predisposing factors : anxiety - dyspnea, palpitations, chest discomfort, numbness and tingling of the hands and around the mouth lasting for several minutes, consciousness is often maintained - slow improvement as hyperventilation ceases
question
Hypoglycemia
answer
- insufficient glucose to maintain cerebral metabolism; secretion of epinephrine contributes to symptoms; true syncope is uncommon - variable precipitating factors including fasting - insulin therapy and a variety of metabolic disorders are predisposing factors - sweating, tremor, palpitations, hunger, headache, confusion, abnormal behavior, coma are prodromal
question
Hysterical Fainting from Conversion Reaction
answer
- brought on through stressful situation - hysterical personality traits are predisposing factors
question
Jacksonian Seizures
answer
- tonic and then clonic movements that start unilaterally in the hand, foot, or face and spread to other body parts on the same side - normal consciousness
question
Other motor focal seizures
answer
- turning of the head and eyes to one side, or tonic and clonic movements of an arm or leg without the Jacksonian spread - normal consciousness
question
Focal Seizures with autonomic symptoms
answer
- a "funny feeling" in epigastrium, nausea, pallor, flushing, lightheadedness - normal consciousness
question
Focal Seziures with subjective sensory or psychic phenomena
answer
- numbness, tingling, simple visual, auditory, or olfactory hallucinations such as flashing lights, buzzing, or odors - anxiety or fear; feelings of familiarity or unreality; dreamy states; fear or rage; flashback experiences; hallucinations - normal consciousness
question
Focal Seizures with Impairment of Consciousness
answer
- the seizure may or may not start with autonomic or psychic symptoms - consciousness impaired and confusion - automatisms included chewing, smacking the lips, walking about and unbuttoning clothes - the patient may remember initial autonomic or psychic symptoms (aura) but is amnesic for the rest of the seizure
question
Focal Seizures that become generalized
answer
- partial seizures that become generalized resemble tonic-clonic seizures; patient may not recall the focal onset - recollection of an aura and unilateral neurologic deficit during the postictal period
question
Tonic Clonic (grand mal) Seizures : Clinical Manifestations
answer
- sudden loss of consciousness sometimes with a cry - body stiffens into tonic extensor rigidity - breathing stops and the person becomes cyanotic - clonic phase of rhythmic muscular contraction follows - breathing resumes and is often noisy with excessive dalivation
question
Generalized Seizures : Postictal State
answer
confusion, drowsiness, fatigue, headache, muscular aching, and sometimes the temporary persistence of bilateral neurologic deficits such as hyperactive reflexes amnesia of the seizure and no recollection of aura
question
Absence Seizures : Clinical Manifestations
answer
sudden brief lapse of consciousness with momentary blinking, staring, or movements of lips and hands but no failing - typical lasts less than 10 seconds and stop abruptly - atypical may last more than 10 seconds
question
Absence Seizures : Postictal State
answer
no aura recalled
question
Myoclonic Seizures : Clinical Manifestations
answer
sudden, brief rapid jerks, involving the trunk or limbs
question
Myoclonic Attack : Clinical Manifestations
answer
sudden loss of consciousness with falling but no movements; injury may occur
question
Myoclonic Attack : Postictal State
answer
either a prompt return to normal or brief period of confusion
question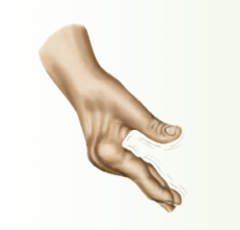
Resting (Static) Tremors

answer
prominent at rest and may decrease or disappear with voluntary movement; common, relatively slow, fine, pill-rolling tremor of parkinsonism, about 5 per second
question
Postural Tremors
answer
appear when affected part is actively maintaining a posture; examples include the fine rapid tremor of hyperthyroidism, anxiety, fatigue
question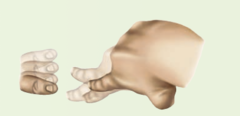
Intention Tremors

answer
absent at rest, appear with movement and often get worse as the target gets closer; include disorders of cerebellar pathways, as in MS, or any other disease of the cerebellum
question
Oral-Facial Dyskinesias

answer
rhythmic, repetitive, bizarre movements that chiefly involve the face, mouth, jaw, and tongue; grimacing, pursing of the lips, protrusions of the tongue, opening and closing of the mouth, and deviations of the jaw
question
Tics

answer
brief, repetitive, stereotyped coordinated movements occurring at irregular intervals i.e., tourette's
question
Dystonia
answer
grotesque twisted postures may result
question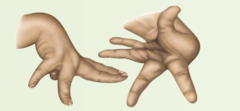
Athetosis

answer
slower more twisting and writhing movements that have a large amplitude; commonly involve the face and distal extremities
question
Chorea

answer
brief, rapid, jerky, irregular, and unpredictable; occur at rest or interrupt normal coordinated movements; they seldom repeat themselves; face, head, lower arms, and hands are often involved
question
Wernicke's Aphasia
answer
- fluent often rapid and effortless speech - inflection and articulation are good but sentences lack meaning and words are gibberish - may be totally incomprehensible - word comprehension, repetition, naming, reading comprehension, writing all impaired - lesion located in posterior superior temporal lobe
question
Broca's Aphasia
answer
- nonfluent - slow with few words and laborious effort - inflection and articulation are impaired but words are meaningful - small grammatical words often dropped - fair word and reading comprehension - impaired repetition, writing, and naming - lesion located in posterior inferior frontal lobe
question
Nystagmus
answer
rhythmic oscillation of eyes; caused by vision impairment early in life, disorders of the labyrinth and cerebellar system, and drug toxicity; can occur normally when watching rapidly moving objects
question
Nystagmus - Lateral Gaze
answer
nystagmus may be present in all directions but only accentuates in deviation of eyes as seen in extreme lateral gaze left or right; normal people show signs of slight nystagmus in lateral gaze
question
Left-beating nystagmus
answer
if eyes jerk quickly to patients left and slowly to the right
question
Pendular nystagmus
answer
nystagmus consisting only of coarse oscillations without quick and slow components
question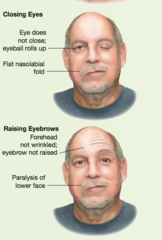
CN VII Peripheral Lesion

answer
paralyzes the entire right side of the face including forehead; right eye does not close and the eyeball rolls up; forehead not wrinkled and eyebrow not raised
question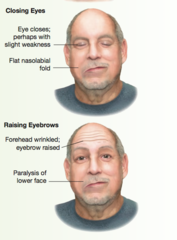
CN VII Central Lesion

answer
Eye closes with slight weakness and forehead is wrinkled with eyebrow raised
question
Lesions Producing Spastic Muscle Tone
answer
Upper motor neuron or corticospinal tract systems
question
Spasticity
answer
- increased muscle tone that is greater when passive movement is rapid and less when passive movement is slow; greater at the extremes or movement arc; sudden limb reflexes - seen in stroke
question
Lesions Producing Rigid Muscle Tone
answer
Basal Ganglion System
question
Lead Pipe Rigidity
answer
increased resistance that persists throughout the movement arc independent of rate of movement
question
Cogwheel Rigidity
answer
rigidity with flexion and extension of the wrist and forearm, a superimpose rachetlike jerkiness seen in parkinson's patients
question
Lesions Producing Flaccid Muscle Tone
answer
lower motor neuron system (from anterior horn cell to peripheral nerves)
question
Flaccidity
answer
loss of muscle tone causing loose and floppy limbs; limbs may be hyperextensible or even flail like seen in Guillain Barre syndrome
question
Lesions producing paratonia muscle tone
answer
both hemispheres, usually in the frontal lobes
question
Paratonia
answer
sudden change in tone with passive ROM
question
Paratonia - Mitghen
answer
sudden loss of tone that increases the ease of motion
question
Paratonia - Gegenhalten
answer
sudden increase in tone making motion more difficult
question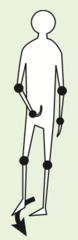
Spastic Hemiparesis

answer
- corticospinal tract lesion in stroke - poor control of flexor muscles during swing phase - arm is flexed, immoble, and held close to side with elbow, wrists, and interphalangeal joints flexed - leg extensors spastic - ankle plantar flexed and inverted - pts may drag toe, circle leg stiffly outward and forward or lean trunk to contralateral side to clear affected leg during walking
question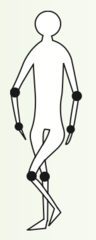
Scissors Gait

answer
- spinal cord disease - caused by bilateral lower extremity spasticity including adductor spasm and abnormal proprioception - stiff gait with slow leg advancement - thighs tend to cross forward on each other with each step - steps are short - pts appear to be walking through water - common in cerebral palsy
question
Steppage Gait
answer
- foot drop - secondary to peripheral motor unit disease - pts drag the feet or light them high with knees flexed and slap them down onto the floor - walking up stairs - cannot walk on heels - tibalis anterior and toe extensors are weak
question
Parkinsonian Gait
answer
- basal ganglia defects - posture is stooped with flexion of head, arms, hips, and knees - pts are slow getting started - short shuffling steps with involuntary hastening - limited arm swings
question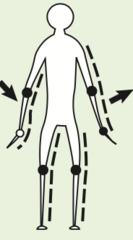
Cerebellar Ataxia

answer
- dx of cerebellum or associated tracts - gait is staggering, unsteady, and wide based with exaggerated difficulty on turns - pts cannot stand steadily w feet together whether eyes are opened or closed - nystagmus, dysmetria, and intention tremor
question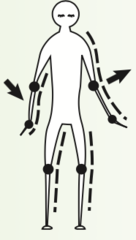
Sensory Ataxia

answer
- loss of position sense in legs - gait is unsteady and wide based - pts throw their feet forward and outward and bring them down first on heels then on toes with double tapping sound - watch grown - with eyes closed they cannot stand steadily with feet together (positive Romberg)
question
Toxic Metabolic Comas
answer
arousal centers poisoned or critical substrates depleted
question
Toxic Metabolic Comas : Respiratory Pattern
answer
if regular may be normal or hypervenilation; if irregular usually Cheyne-Stokes
question
Toxic Metabolic Comas : Pupillary size and reaction
answer
- equal and reactive to light - pinpoint = opiates/cholinergics; need magnifying glass to see reaction - fixed and dilated = anticholinergics/hypothermia
question
Toxic Metabolic Comas : Causes
answer
- uremia - hyperglycemia - alcohol - drugs - liver failure - hypothyroidism - hypoglycemia - anoxia - ischemia - meningitis - encephalitis - hyperthermia - hypothermia
question
Structural Coma
answer
lesion destroys or compresses brainstem arousal areas either directly or secondary to more distant expanding mass lesions
question
Structural Coma : Respiratory Pattern
answer
- irregular especially Cheyne-Strokes or ataxic breathing
question
Structural Coma : Pupillary Size and Reaction
answer
- unequal or unreactive to light - midposition, fixed = midbrain compression - dilated, fixed = compression of CN III from herniation
question
Structural Coma : Causes
answer
- epidural, subdural, or intracerebral hemorrhage - cerebral infarct or embolus - tumor or abscess - brainstem infarct, tumor, or hemorrhage - cerebellar infarct, hemorrhage, tumor, or abscess
question
Glasgow Coma Scale
answer
higher number = more aware
question
Bilaterally Small Pupils

answer
- 1-2.5 mm - suggest damage to the sympathetic pathways in the hypothalamus or metabolic encephalopathy - diffuse failure of cerebral function that has many causes including drugs - light reactions are usually normal
question
Pinpoint Pupils
answer
- <1mm - suggests a hemorrhage in the pons or the effects of morphine, heroin, or other narcotics - light reaction may be seen w magnifying glass
question
Midposition Fixed Pupils

answer
- slightly dilated and fixed to light - suggest structural damage in the midbrain
question
Bilaterally fixed and dilated pupils
answer
- may be due to severe anoxia and its sympathomimetic effects as seen after cardiac arrest - may also be seen from atropinelike agents, phenothiazines, or tricyclic antidepressants
question
Bilaterally large reactive pupils
answer
may be due to cocaine, amphetamine, LSD or other sympathetic nervous system agonists
question
One Large Pupil
answer
herniation of the temporal lobe causing compression of the oculomotor nerve and midbrain; most commonly seen in diabetic pts with infarction of CN III
question
Decorticate Rigidity (Abnormal Flexor Response)
answer
- upper arms are flexed tight to the sides with elbows, wrists, and fingers flexed - legs are extended and internally rotated - feet are plantar flexed - implies a destructive lesion of the corticospinal tracts within or very near the cerebral hemispheres - when unilateral = chronic spastic hemiplegia
question
Hemiplegia (Early)
answer
- sudden unilateral brain damage involving the corticospinal tract - one-sided paralysis - flaccid in early course with spasticity developing larger - paralyzed arm and leg are slack falling loosely without tone - spontaneous movements or responses are limited to opposite side - leg may lie externally rotated - one side of lower face is paralyzed and that cheek puffs on expiration - both eyes may be turned away from paralyzed side
question
Decerebrate Rigidity (Abnormal Extensor Response)
answer
- jaws are clenched and neck is extended - arms are adducted and stiffly extended at the elbows with forearms pronated, wrists and fingers flexed - legs are stiffly extended at the knees with feet plantar flexed - may occur spontaneously or only in response to external stimuli (light, noise, or pain) - caused by a lesion in diencephalon, midbrain, or pons OR by metabolic disorders such as hypoxia and hypoglycemia



